With my 20th PT Class Reunion coming up this year, I’ve been feeling a little nostalgic—reflecting on the good old days of Gross Anatomy lab, the camaraderie with classmates, and an abundance of time dedicated to establishing a foundation in physical therapy. One of the fundamentals we learned, of course, was how to assess correct posture. We had plumb lines that ran from the ceiling, memorized the four postural types as described by Florence Kendall, and recorded them on our worksheets.
Then, browsing Twitter I came across this interesting tweet from Peter O’Sullivan looking at the term “derangement.”
The word derangement be abandoned to negate the
tendency to link the word to structural pathology or vulnerability.https://t.co/WYnR7Uxp1P pic.twitter.com/wWbiX0A2ir— Peter O’Sullivan (@PeteOSullivanPT) February 4, 2017
And when I read Effects of stretching exercises for posture correction: systematic review, I found myself asking: is there such a thing as “good posture?”
Harkening back to our PT school days, good posture was an absolute certainty. But, practicing over two decades and factoring in homeostasis, human nature, natural aging and gravity, I conclude that good posture is actually a misnomer.
Webster defines posture as “the way in which your body is positioned in sitting and standing.” As a profession, we have decided to ask patients to find equilibrium in statics. But for a healthy neuromuscular system, it is equilibrium in dynamics that is essential. There are many other biopsychosocial benefits to dynamics. To summarize, we require a requisite number of repetitions in each joint to provide adequate nutrition to the articular cartilage, provide appropriate signaling to the neuromuscular system through the central nervous system expanding cortical representation of normal function, (which I addressed in It’s All About Balance.)
In this study, Nunes Da Silva Filho, et. al. could not make a conclusion nor establish a consensus if posture correction could be obtained with appropriate stretching exercises. They only found five research articles and two dissertations to review for their publication. Why is there such a dearth of research? Are we asking the right questions? Should we seek out the absolute best posture for each patient? Asking them to assume a static position and hold it while sitting makes as much sense as asking them to maintain full elbow extension all day long, because that is good posture.
The elbow is a fascinating joint complex and very few operative replacements are performed (1.4/100000 compared to ~80/100000 for hip replacements). The replacements I have seen clinically have been a result of trauma or rheumatoid arthritis. Why would this be? Outside of the fact that it is a technically arduous procedure, I believe that through habitual movements, the elbow (through eating, reaching, dressing, washing, etc.) can maintain optimal neuromuscular and articular health.
The questions asked in the above article appears simple. Enter any PT practice and posture correction is a foundation of treatment. When a PT walks into the waiting room, their patients are sitting up straight, hoping they will be credited for their “good posture”. But, the next time you are correcting posture, ask yourself about the purpose behind this instruction.
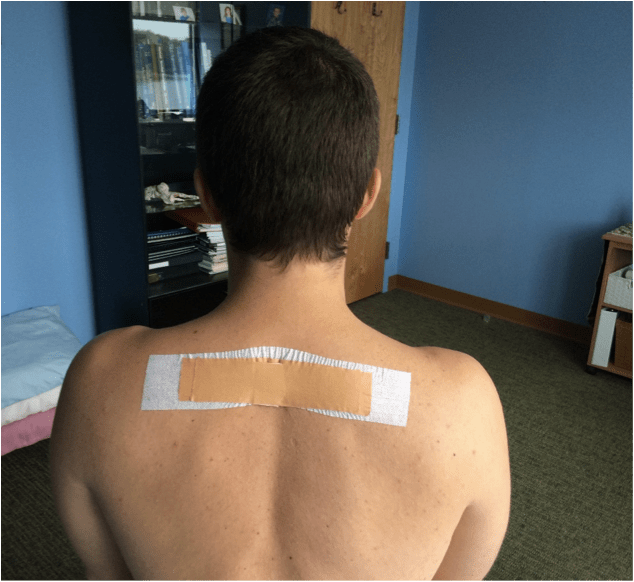
Let us see if we can create a new paradigm of movement in posture. This photo is an example of using tape to increase a patient’s awareness of posture.
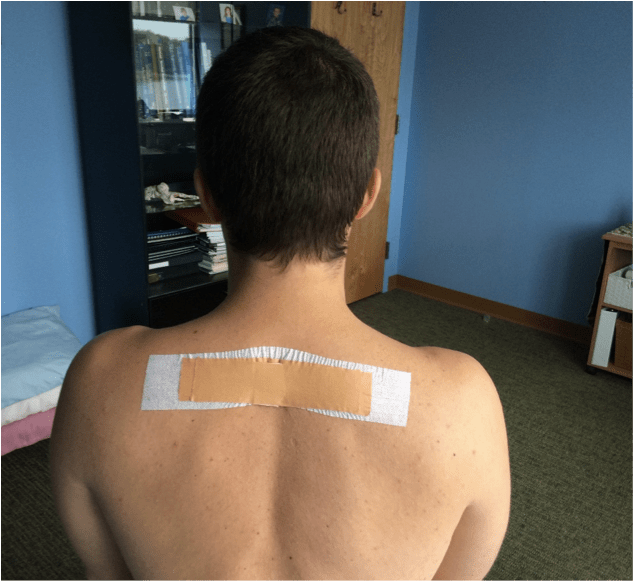
Applying dynamics to posture may offer a better foundation for research than our current static model. As David Butler states, let’s take the best of research, our patients and ourselves, and apply it to clinical practice.
What do you think? Join me in sunny Orlando, Florida for Lumbopelvic Spine I or at one of our other upcoming manual therapy courses.

*Abstract of the Week Shared by NAIOMT instructor Terry Pratt, MS, PT, COMT, FAAOMPT